FAQ
We will file an insurance claim on your behalf to the primary insurance on file. If there is a secondary insurance on file, we will also file a claim for the amount not paid by your primary insurance. If there is no secondary insurance on file, you will receive a bill for any co-payment or deductible as determined by your primary insurance company.
If your insurance company sends payment directly to you, you may either endorse the check or write a personal check addressed to us for that amount received and mail the check to our business address below.
Reston Anesthesia Associates, P.C.
607 Herndon Parkway Suite #101
Herndon, VA 20170
Column 1: Dates
The first line item will be the date of service. All other line items will be the date a payment or adjustment was taken.
Column 2: Description of service
This is where you see the service billed for, the provider who performed the service, and any information regarding payments and adjustments.
Column 3: Financial Amounts
These are the costs for what is described in column 2.
Columns 4 & 5: Balances
These are any balances on your account to be paid by your insurance (Column 4) or you (Column 5).
EXAMPLE STATEMENT:

Your EOB is specific to your insurance company. Remember that your EOB is not a bill, it just explains what was covered by your insurance plan.
Your EOB may identify:
- The patient and the service provided
- The amount charged by the provider
- The amount of the charges that are covered and not covered under your plan
- The amount paid to your provider
- The amount you're responsible for Your provider may bill you separately for any charges you're still responsible for. You may receive more than one EOB over time, this indicates that your initial claim has been denied and was appealed. Denials and Appeals can have numerous reasons and are generated by our office. Rarely, we may correspond with you to help us in this process.
Remember that your EOB is not a bill, it just explains what was covered by insurance. Your provider may bill you separately for any charges you're still responsible for. You may receive a few EOBs over time if your claim is being appealed.
Sample EOB
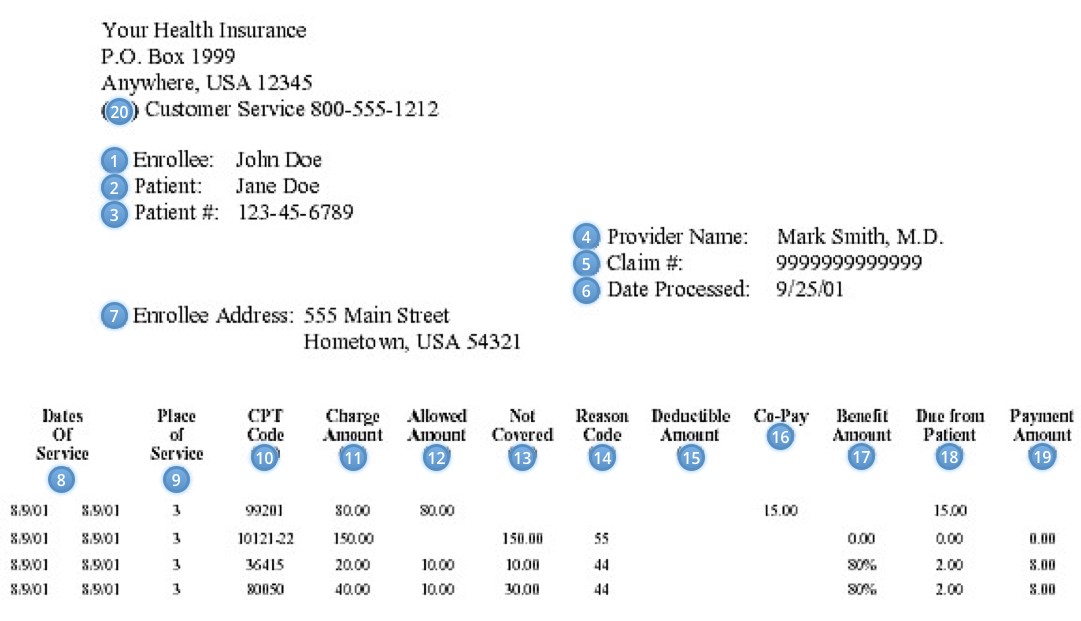
- Enrollee Name: Identifies the policyholder.
- Patient: Identifies the patient.
- Patient #: Identification number for the patient.
- Provider Name: Identifies the name of the doctor or facility billing for the services.
- Claim #: A number assigned to the claim by the insurance company for processing.
- Date Processed: Date the claim is processed.
- Enrollee Address: Indicates the address of the enrollee; this should be verified with each claim. Wrong addresses can cause problems in claims payment.
- Dates of Service: The date the service was rendered.
- Place of Service: The location the service was provided.
- CPT Code: This identifies the service performed. This code is universal and dictates the payment allowances.
- Charge Amount: Amount charged by your provider for their service.
- Allowed Amount: Amount determined by a preset regional schedule of "usual and customary" (UCR) charges.
- Not Covered: Amount not included in the allowed amount; usually this is the amount deemed over the usual and customary allowance. This amount can become the patient's responsibility.
- Reason Code: This is an explanation of why a service or amount has been denied.
- Deductible: A contractual amount determined by your insurance amount that is the patient's responsibility. Refer to your schedule of benefits.
- Co-Pay: A contractual amount specific to your plan that can actually exceed your deductible amount and continue until a "maximum out of pocket" amount is satisfied as determined in your plan. Refer to your schedule of benefits.
- Benefit Amount: The percentage of the amount covered that will be paid by your plan. The percentage paid will be determined by your schedule of benefits.
- Due from Patient: The amount the patient is responsible for paying to the provider. This generally includes the co-insurance amount and deductible.
- Payment Amount: The amount paid to the provider.
- Customer Service: This is the number used to contact your insurance provider's customer service.
A procedure can have numerous separately billable components.
- The professional services of the surgeon/proceduralist
- The professional services of the anesthesiologist and/or a certified registered nurse anesthetist (CRNA)
- The facility fee (hospital or surgery center)
- Pathology/lab fees
- Radiology fees
Each of these services are usually provided by separate medical groups, facilities and or companies which have no business ties and are contractors to the facility.
We only submit bills for anesthesia services.
No. Anesthesia services are often provided by a certified registered nurse anesthetist (CRNA) and supervising physician anesthesiologist. Insurance providers simply require that the anesthesia services bill be submitted to them with the entire charge split between the crna and anesthesiologist.
